Plantar heel pain or 'Fasciitis'
The dreaded stab to your heel when you first get up.
Now there are several causes of heel pain. However, I am going to focus on one injury in particular…
Plantar Fasciopathy
(Commonly referred to as Plantar fasciitis/ fasciosis, plantar heel pain, or ‘bloody sore’ foot!)
This is a condition that, whenever I mention I’m a podiatrist, a story of someone’s ordeal seems to arise shortly after.
I’ve heard every treatment and theory. From jumping off a table and snapping it (The “Robert Harvey” method) to the old school iced water bottle roll.
Yet not to worry, I’m going to give you an insight into the big 80% ‘s. The key pillars and long term bang-for-your-buck strategies of how to get on top of plantar fasciopathy.
So let’s start with some basics…
What is the Plantar Fascia?
Fundamentally the plantar fascia is connective tissue underlying the bottom of the foot.
The simplest analogy is to imagine a strong, thick rubber band like structure which runs from the base of your heel to the knuckles or ball of your foot.
When we walk, and in particular when we propel (push) forward off our toes, the plantar fascia is put under tension and pulled. This is great, as it helps to provide structure to the foot in a really energy efficient manner.
What is Plantar Fasciopathy?
Plantar fasciopathy refers to the occurrence of pain through the connective tissue of the plantar fascia, typically surrounding its insertion to the heel bone, on the background of overuse.
Unfortunately, this is an extremely common issue, particularly in those who are active. This form of heel pain finds itself as the 3rd most common injury impacting runners. Further investigations suggest that approximately 10% of people are affected by this pain.
How is it Diagnosed?
Typically diagnosis can be made without imaging by an appropriately skilled health practitioner such as your podiatrist or physiotherapist. This can be done through analysis of specific symptoms, activity and injury history in combination with gait and biomechanical assessments.
Below are a couple of common characteristics and findings that can be used in combination with the above clinical examination to confirm this diagnosis.
Imaging:
- Plantar fascia tissue which is greater than 4mm thickness upon imaging
- Abnormal tissue structure throughout the fascia (such as tear, lesion (ie.fibroma), scarring)
Symptoms:
- Pain in the central to medial portion of heel bone underneath foot.
- Pain post rest into initial weight-bearing
- Reduction in symptoms when completing lower intensity activities for short periods
- Flare in symptoms during prolonged or higher intensity activities
What causes Plantar Fasciopathy?
Simply, overload of the structure and tissue from loading. Traditionally this comes in two main forms:
- Tensile loading
This is where the fascia is being pulled. An easy analogy is to go back to our strong rubber band. Here with each step we take we are pulling and stretching the fascia. Typically it loves this. However if it has to undertake too much of this pulling in comparison to what it can handle, then symptoms can arise.
- Compressional loading
This is where the fascia experiences twisting or squeezing. From our analogy imagine the rubber band being pulled and now twisted. This is the loading that the fascia doesn’t like as much and therefore can’t tolerate as much. Therefore takes a lot less compressional loading to cause pain.
The reasons for the increase in these two forms of load can come from a variety of reasons. A couple of the main contributing factors are:
- Decreased capacity of lower leg & foot musculature
- Decreased ankle joint range
- Spike in higher intensity or prolonged duration activity
- Change in footwear to more demanding selections
- Foot posture affecting rates of loading
How do we treat it?
Deloading
Our main aim here is to reduce symptoms by removing the aggravating load to the plantar fascia.
We can do this through:
- Footwear
Here we focus on picking specific footwear characteristics based on the biomechanical factors which are contributing to the overload of the plantar fascia.
A major factor here is typically around the torsional stability (the flexibility) of footwear. Generally the more flexible, the greater the demands on the stabilising musculature and structures of the feet and lower limb. Therefore the more load to the plantar fascia.
Now flexibility isn’t a bad thing, however if we have a structure that is injured due to exposure to high loads, then initially addressing this is crucial.
- Orthotics
There is strong evidence for the use of custom orthotics in the treatment of plantar fasciopathy.
This is because a custom orthotic can be really specific in the reduction of load, whether this be compressional or tensile, going through the plantar fascia and therefore directly helping to provide a considerable easing in symptoms.
- Taping
A great short term intervention similar to the above which allows for specific rates of movement to be slowed and specific loading types to be mitigated.
Significant evidence suggests that taping is successful in providing pain reduction for the initial stage of treatment and indicates that orthotics are likely to be beneficial to decrease pain.
- Activity modification
Although this is something that we attempt to avoid, in the short term, removing higher intensity or longer duration aggravating activities is an effective measure to settle symptoms.
It is then with symptoms settled that we can then turn to improving capacity, function and strength and set in place a place to re-introduce previously aggravating activities.
Re-loading
Here we are aiming to increase the capacity, and therefore ability for the fascia to tolerate load post symptom reduction.
Strength & conditioning exercises
These two are fantastic initial exercises to start to build strength throughout the stabilsing structures and initially load the fascia.
- Calf & intrinsic foot strength
2 key exercises:
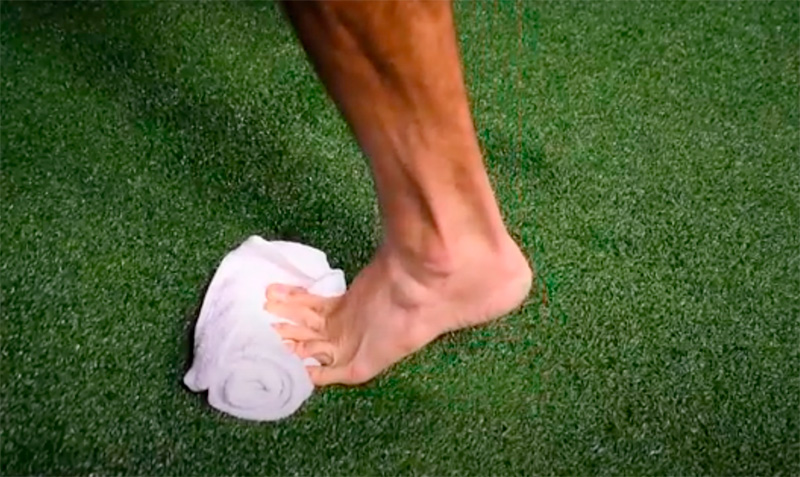
Single leg Calf raise isometric hold
– With folded towel under toes & forefoot
– Slight lean into wall
– Up through big toe & hold
– x 45 sec
– Then coming down slowly
– Have a 30 sec break between sets
– Repeat 5 times
Big toe yoga (Big toe flexor strength)
– Standing with feet flat on the ground
– Allow the big toe to come up, nice and tall (while the foot stays on the ground)
– Drive the big toe down to the floor
– Remember to keep the little toes long and loose
– No clawing at the ground with little toes
– x 20

Other short term symptom management can involve:
- NSAIDs (non-steroidal anti-inflammatory drugs)
- Soft tissue massage & Joint mobilization techniques
- ESWT (Extracorporeal Shock Wave Therapy)
- Cortisone injection
If you have any questions, please feel free to get in touch with Angus McSweyn or book an appointment so we can get you back doing what you love pain free!
Angus McSweyn is a Sports Podiatrist who consults at Complete Balance Physiotherapy (Tullamarine Clinic) located at the Essendon Football Club.
Nick Kane is a titled Sports & Exercise Physiotherapist and the current Head Physiotherapist at the Essendon Football Club. Holding a Master of Sports Physiotherapy, Nick specializes in elite-level rehabilitation for hip and groin pain, recurrent hamstring injuries, and post-surgical recovery. He brings his expertise in professional sports to our Maribyrnong and Tullamarine clinics to help patients achieve high-performance results.
